The effects of stroke can leave one side of your body paralyzed or weakened. This poses challenges to your independence.
Problems with muscles
Stroke can affect muscles in your arms, legs, hands and feet. After a stroke, the muscles may become limp and feel heavy (flaccid or low tone). In the weeks or months after a stroke, the muscles may shorten and become very tight, making them more difficult to move. This is called spasticity (high-tone).
These changes in muscle tone can affect joint stability and movement. Low muscle tone around the shoulder joint can lead to shoulder subluxation — a partial dislocation of the shoulder joint. It is very important to handle, move and position an affected limb carefully to help avoid injury to joints, muscles and ligaments. Talk to your healthcare team about proper positioning and strategies to help prevent injuries and promote recovery.
Changes in muscle tone, movement and control can also lead to a stiff, swollen and painful shoulder, hand or wrist.
Treatment may involve:
- occupational therapy
- physiotherapy
- gentle handling
- proper positioning
- exercises
- botulinum toxin injections
- splints or orthotics – special devices that help position and support joints (note: routine use of upper extremity splints is not recommended although a person may be fitted with a splint in some situations).
Muscle spasticity in the hand may lead to finger and hand tightness, causing the hand to close into a tight fist. It is important to make sure the hand stays clean and dry, and that the nails are well trimmed. Good hygiene can prevent skin damage. Talk to your healthcare team about the best way to manage spasticity and take care of the tightness in your hand.
Where to get support
The member of your healthcare team who can help may include a:
- physiatrist (rehabilitation doctor)
- occupational therapist
- physiotherapist
- nurse.
Getting around (mobility)
Getting around your home and community is an important part of your independence. After a stroke, muscle, strength and balance problems may make it hard to get around independently. Some people may need assistive devices such as a walker or wheelchair. No matter how you get around, it is important to keep safe.
Mobility aids
A mobility aid is any assistive device that helps you get around. Make sure it meets your needs, both inside and outside of your home. All devices need to be fitted to you. You will also need instructions on how to use them safely. Your physiotherapist or occupational therapist can help with this.
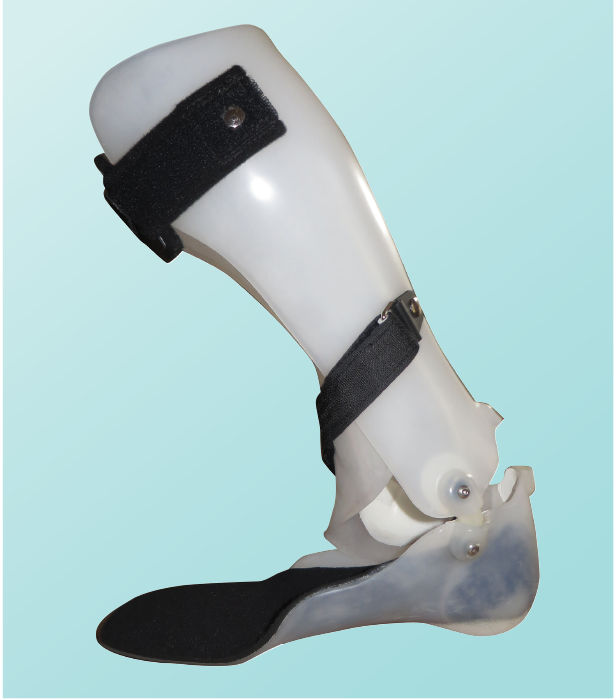
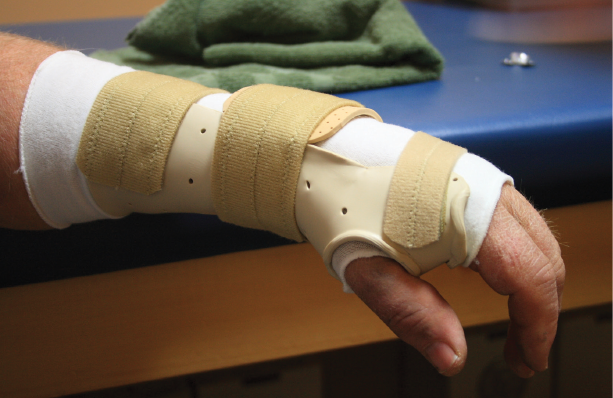
Orthotics and braces
Orthotics or braces can help to support and stabilize muscles that have been weakened or developed spasticity after a stroke. They can support and stabilize the limb to help it function.
Walkers
Walkers can provide you with support when walking. Some have no wheels, two wheels or four wheels. Your physiotherapist will make sure you get the one that is right for you and will show you the correct posture when using it.
Canes
There are different types of canes. Some have a single prong at the end. Some canes are balanced with three prongs. Some have a rubber tip, with a claw you can attach for walking in winter.

Wheelchairs
If you need a wheelchair, you will be fitted by a member of your healthcare team with a chair that meets your physical and practical needs and fits into your home environment. They will show you how to sit properly and check to see if you need a seat cushion or back rest. Proper positioning will help to prevent injuries and pressure sores. You will need to learn to transfer or move safely from your wheelchair to the toilet, bed or another chair.
You will also need to plan how to get around your home in the wheelchair. Is there enough room to pass through doorways and turn around?
Make sure that your wheelchair has a seatbelt — and use it. A team member will help you learn how to transfer in and out of the chair safely.
An electric scooter may be an option for you.
Where to get support
Your occupational therapist and physiotherapist will help you choose and fit your mobility devices. They will train you to use them safely.
Provincial or private insurance plans may fund mobility devices.
Local service groups sometimes lend equipment.
Related information
Take a look at the Everyday tasks section for practical tips to adapt your daily activities.
Upper extremity management after stroke (video)
