What is heart valve surgery?
Heart valve surgery and procedures are performed to repair or replace a valve in the heart that is not working properly because of valvular heart disease (also called heart valve disease). Heart valve surgery is open-heart surgery through the breastbone, into the chest. It is a major operation that can last two hours or longer and recovery often takes several weeks. There are newer, less invasive procedures suitable for some types of valvular heart disease, but they are only done at certain hospitals.
Why is it done?
In a healthy heart, valves control the flow of blood by making it move in one direction through the heart and the body. If a valve is not working correctly, blood flow and the delicate network of blood vessels that carry oxygen throughout the body are affected.
If your valve problem is minor, your doctor may monitor your symptoms or treat you with medication. If your condition is more serious, surgery is usually required to repair or replace the valve to prevent any lasting damage to your heart valve and your heart.
What is done?
Depending on the problem, there are several different procedures for repairing or replacing valves.
1. Surgical valve repair
Surgical procedures are generally used for problems with the mitral or tricuspid valves.
- Commissurotomy is a treatment for a tight valve. The valve flaps (leaflets) are cut to loosen the valve slightly, allowing blood to pass easily.
- Annuloplasty is done for a leaky valve. There is a ring of fibrous tissue at the base of the heart valve called the annulus. To repair an enlarged annulus, sutures are sewn around the ring to make the opening smaller. Or, a ring-like device is attached around the outside of the valve opening to support the valve so it can close more tightly.
- Valvulotomy is a procedure to enlarge narrowed heart valves. It can also be done with the help of a balloon.
2. Non-surgical valve repair
Percutaneous or catheter-based procedures are done without any incisions in the chest or stopping the heart. Instead, a thin flexible tube called a catheter is inserted into a blood vessel in your groin or arm and then threaded through the blood vessels into your heart.
- Percutaneous or balloon valvuloplasty/valvotomy is used for stiffened or narrowed (stenosed) pulmonary, mitral or aortic valves. A balloon tip on the end of the catheter is positioned in the narrowed valve and inflated to enlarge the opening.
- Percutaneous mitral valve repair methods - such as edge-to-edge repair - can fix a leaky mitral valve in a patient who is considered high risk for surgery. A catheter holding a clip is inserted into the groin and up into the left side of the heart. The open clip is positioned beyond the leaky valve and then pulled back so it catches the flaps (leaflets) of the mitral valve. Once closed, the clip holds the leaflets together and stops the valve from leaking.
3. Heart valve replacement
If your heart valve is too badly damaged to be repaired, surgery may be needed to replace it with a new mechanical or biological valve. Age is generally a factor in deciding which type to use – biological valves are generally preferred for older people. You and your doctor will discuss the options and decide which is best for you and your circumstances.
- Mechanical valves made of long-lasting metals, carbon, ceramics and plastic were the first to be used in valve replacement surgery. They have been refined and improved since being introduced in the 1960s.
- The major advantage of a mechanical valve is durability – they can last a long time.
- A fabric ring is used to sew the valve to heart tissue.
- Mechanical valves can lead to blood clots which may in turn cause a heart attack or stroke. To prevent clots, people with mechanical valves must take blood-thinning medications (anticoagulants) every day for the rest of their lives. This can have implications for women of childbearing age or for people who have a history of major bleeding. Depending on the type of blood thinners, you may require routine blood-testing to monitor your INR (international normalized ratio) to measure your blood’s tendency to clot.
- A mechanical valve makes a soft clicking sound when it closes. This can bother some people.
- Biological (also called bioprosthetic) or tissue valves are specially prepared natural valves that come from human donors or animals.
- Animal source valves (a xenograph) – usually cows or pigs – are similar to valves in the human heart. They are tolerated well and are less likely to form blood clots than mechanical valves.
- Human heart valves from a donated heart (an allograft or homograft) are tolerated well and tend to last longer than animal valves. Using human valves is uncommon.
- Valves can come from your own tissue (an autograft). In a Ross (or switch) procedure, your functioning pulmonary valve is used to replace your damaged aortic valve. Your pulmonary valve is then replaced with a donated one.
- People with biological valves need to take blood thinners in the short term.
- Biological valves are not as durable as mechanical valves. They are more durable in the aortic position and in older patients.
4. Minimally invasive valve repair and replacement
Unlike conventional surgery, minimally invasive surgery does not involve sawing through the breastbone and opening the chest. It doesn’t require stopping your heart or using a heart-lung machine. The surgeon watches your heart on a video screen and operates using long-handled surgical tools inserted through small incisions. In some cases, robotic arms are used. Minimally invasive valve repair and replacement is suitable for some types of valvular heart disease, but is only available in some hospitals. It may also be called endoscopic or robotic heart surgery.
- Transcatheter aortic valve implantation (TAVI) is also called transcatheter aortic valve replacement (TAVR). TAVI is a minimally invasive surgical valve replacement procedure that is used to treat symptomatic aortic valve stenosis, with two key differences from traditional valve replacement surgery. Rather than opening up the chest, TAVI is done through small incisions in the groin or chest. Instead of repairing, or removing and replacing the damaged aortic valve, a new aortic valve is implanted directly on top of the damaged one.
- The surgeon inserts a catheter containing a new, collapsible aortic valve through small incisions in the groin or chest.
- Using ultrasound and chest x-rays, the catheter is guided to the correct position in the heart and the new valve is implanted and expanded.
- Once the new valve is in place, it starts to control blood flow immediately.
- People who undergo TAVI tend to recover faster and have shorter hospital stays (average three to five days) than people who have open-heart valve surgery.
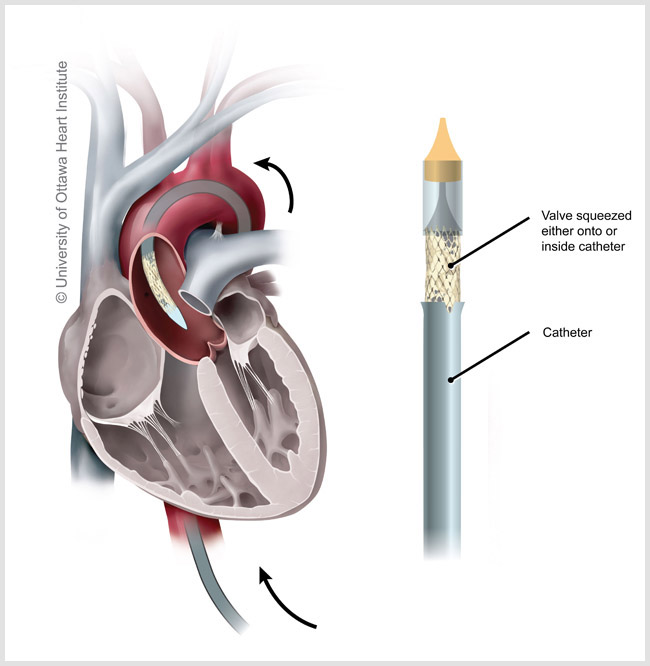
TAVI is usually considered for people who are at high risk for complications from open-heart surgery. Your healthcare team will assess your symptoms and overall health to determine if TAVI is an option for you.
What you can expect?
Before the procedure
If you smoke, you should stop at least two weeks before your surgery. Smoking can contribute to blood clotting and breathing problems.
Approximately a week before your surgery, you may be asked to visit your hospital’s pre-admission unit. The risks and benefits of the procedure will be explained to you and you will be asked to sign a consent form. At this appointment, tests may include:
- blood work
- urine sample
- electrocardiogram (ECG)
- chest X-ray
Please inform your healthcare team if you:
- Have ever had a reaction to any contrast dye, iodine, or any serious allergic reaction (for example, from a bee sting or from eating shellfish).
- Have asthma.
- Are allergic to any medication.
- Have any bleeding problems or are taking blood-thinning medication.
- Have a history of kidney problems or diabetes.
- Have body piercings on your chest or abdomen.
- Have had any recent change in your health.
- Are – or may be – pregnant.
Most patients are admitted to the hospital the day before their procedure. The night before, you will be asked to bathe to cleanse or disinfect your skin. Preparation for surgery may include:
- Washing the area to be operated on with an antiseptic cleanser.
- Clipping the hair on your chest.
- Not eating or drinking after midnight to reduce the risk of vomiting while you are unconscious.
During the surgery
Surgical valve repairs and replacements are done under a general anesthetic so you will be asleep throughout the operation.
During conventional surgery, the surgeons will stop your heart while they work on the valve or valves. You will be hooked up to a heart-lung machine that takes over the pumping action of your heart, so that your body continues to receive a flow of oxygen-rich blood.
- The surgery will take at least two hours or longer, depending upon the number of valves that need to be repaired or replaced.
- You will wake up in the recovery room or an intensive care unit (ICU).
- You will stay in the hospital for about a week.
- How quickly you recover from surgery will partly depend on how healthy you were before the surgery.
If you have minimally invasive surgery, your heart will not be stopped and a heart-lung machine will not be used. Your hospital stay will probably be shorter and your recovery quicker than conventional open-heart surgery.
Going home
When you return home, keep an eye on your incisions. Some bruising is normal, but contact your doctor if you experience:
- increased pain
- redness
- swelling
- bleeding
- draining from an incision
- fever
- chills
- generally feeling unwell.
Cardiac rehabilitation
Cardiac rehab is a personalized program of exercise, education and counselling to help you recover from heart valve disease. Rehab will help you regain your strength and reduce your risk of having other heart problems in the future. Talk to your doctor about how to find a program in your area or contact your public health department or hospital. The Canadian Association of Cardiac Rehabilitation also has a cardiac rehabilitation program directory to help you find a program in your community.
Lifestyle changes can help
Healthy choices can help you manage heart disease. Get practical tips and advice from Heart & Stroke experts on how to get healthy. Learn how to:
Talk to your healthcare provider about the lifestyle changes that will benefit you the most.
Related information
Watch our valvular heart disease webinar to hear researchers and people living with the disease discuss its causes, symptoms and treatment.
The Heart Center at St Paul’s Hospital in BC offers resources and information on heart valve procedures.
HealthLinkBC also offers resources and information.
The Ottawa Heart Institute produces a patient and family guide that talks about preparing for the procedure, what to expect in the hospital, going home and tips for living with your new aortic valve.
What you can expect after your heart surgery from Hamilton Health Sciences outlines some typical things that you can expect while you are in the hospital.
Special thanks Updates to this health information content are made possible through an unrestricted educational grant from Edwards Lifesciences (Canada) Inc. This publication has been independently researched, written and reviewed by Heart & Stroke. Edwards Lifesciences (Canada) Inc has no direct influence over any aspect of the content and educational activities funded by this grant.
