
A love story saved
Donna and Barry beat heart disease together. Now they’re taking care of their health and spending more time with their family.
Chapter 1 A dire prognosis
“You are having a heart attack right now,” doctors told Donna Hart in the emergency department. The team finally managed to get her heart under control, but they could find no sign of the blood vessel blockages that trigger most heart attacks.
That was December, 2014. After eight days in intensive care, Donna heard the words heart failure for the first time. She struggled to understand the diagnosis. At 57, she worked full-time as a social worker and was fitter than many 20-year-olds.
She shares a passion for physical activity with her husband, Barry Tsuruda. Together they logged thousands of kilometres on their bikes each year, with local cycling groups near their home in Milton, Ont. Donna swam laps twice a week with a masters club the rest of the year, and she was proud of her washboard abs.
But starting that fall, she had been feeling tired and out of breath. She assumed her fitness had just taken a dip. She trimmed her briefcase to the bare essentials so she’d be less out of breath as she walked from her car to the office. She would even hold her breath so no one would see how she struggled.
Eventually Donna got a diagnosis of heart failure caused by giant cell myocarditis, a rare type of inflammation of the heart with a dire prognosis: Most people survive only five months without a new heart. Donna’s heart was functioning at just 30% capacity, so her organs and muscles were not getting all the oxygen and nutrients they needed.

Donna and Barry with their son Ryan, daughter in law Jennifer, and granddaughter Ada at a Halloween event.
Chapter 2 Two weeks to live
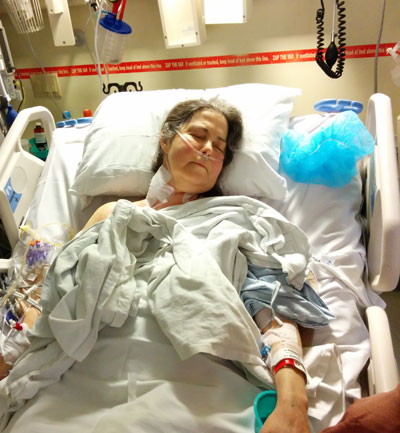
Donna’s health went downhill fast. She was sent to the Peter Munk Cardiac Centre at Toronto General Hospital, where tests revealed her heart function had fallen even further, to 13%. “Three weeks earlier, I had 30%,” she says. “I’m not a math whiz, but I could figure out I had two weeks to live.”
She went home with a defibrillator and was soon given a blood pressure cuff that automatically sent messages back to her healthcare team.
“We immediately went to get our wills done, get our house in order,” Donna says. “That was very, very hard for Barry. But I wanted to get these tasks done, to know I wasn’t leaving a mess for him.”
Soon Donna was back in hospital. “If you leave again, your other organs will fail, and you will have to go into palliative care,” her doctors told her. Only a heart transplant would save her life.
So the wait began for a new heart. As winter turned to spring and Donna got sicker, she tried to stay positive for Barry and their two children, Kaitlyn and Ryan. When they visited her in hospital, she told them she was sure a new heart would arrive by Mother’s Day.
Then one spring day, Barry was out for a 25-km ride with his cycling club. “About halfway through, I felt really, really tired,” he recalls. “I actually lay down on the side of the road to rest. Then I rode the 10 km back to where I had parked and drove home.”
Luckily, Kaitlyn was there. She took him to emergency, where nurses told Barry, “You’re having a heart attack.”
Barry had surgery to implant five stents in his blocked arteries, spending five days in intensive care. With both parents in hospital, Ryan had to take on power-of-attorney for both. That was hard for the family, but the couple managed to keep smiling as they texted each other pictures comparing their hospital meals.
Finally, less than a week after Barry’s surgery and one day after Mother’s Day, the family got the news they wanted: There was a heart for Donna.

Donna and Barry love taking their granddaughter, Ada, to the zoo.

Donna’s new heart has brought her a lot of vitality.

Heart disease has affected their entire family, so Donna and Barry are grateful for the treatments that keep them alive and active.
Chapter 3 Getting back on her bike
Every year about 180 adult heart transplants are performed in Canada. For patients like Donna, with end-stage heart failure, it’s the only cure. Research has greatly improved outcomes since 1968, when Canada’s first heart transplant was performed.
While it’s miraculous, a heart transplant is not, for most patients, a ticket back to their old lives.
Dr. Sharon Chih is a cardiologist specializing in heart transplant. With support from Heart & Stroke donors, she is researching ways to improve outcomes by earlier detection of a complication called cardiac allograft vasculopathy or CAV. It affects up to half of heart transplant patients within 10 years.
For Donna, recovering after the transplant took time. “They tell you it’s a tough first year, but I found it was a tough 18 months,” she says. She slowly regained her strength, starting with short walks; by June, she was riding her bike around the block. In fact, she and Barry have become regular participants in Heart & Stroke Ride for Heart each June, raising funds for life-saving research.
Determined to do anything to maintain their health, Donna and Barry now have annual visits to their cardiologists.
“My heart function is really good now,” Donna says. “With my last echocardiogram, my heart function was at 61%. That’s good because 60% is considered normal.”
Barry’s experience of having a heart attack without pain (just debilitating fatigue) has helped others recognize the signs of heart attack and advocate for themselves to get the care they need.
Marking 39 years of marriage, the couple has a lot going on. They’re keeping active and outdoors, cycling, hiking, camping and fishing, like they’ve always done. Their daughter, now Dr. Kaitlyn Tsuruda, completed her PhD in Epidemiology. Their son Ryan and his wife have started a family - a daughter, Ada - and a baby on the way. “Being a grandparent is so much fun,” Donna says. They’re certainly glad they haven’t missed any of it.
Donna and Barry have each beaten heart disease once. And together they’re determined to stay strong as a family— in case they need to beat it again.
- Learn more about recovering from heart disease.
- Know the signs of heart attack.

Join the fight to end heart disease and stroke.
Related stories

Extending heart health for aging
Dr. Susan Howlett targets frailty to help you live healthier, longer. Especially women.

Samantha’s fight for every word

Preventing stroke before it strikes
Research by Dr. Jodi Edwards could head off the factors that increase risk – especially for women
