Exercise is one of the most important things you can do for your heart health. Physical activity helps you live longer and reduces the risk of dying from heart disease by 50 per cent.
But after you’ve been diagnosed with heart disease, you may feel scared and uncertain. Where do you start? How much activity is healthy and safe?
Living Well with Heart Disease is a new book from the Heart and Stroke Foundation, for people with heart disease and their families. Written by experts, it’s a guide to every aspect of recovery, from medications through dealing with the emotional impact. You can download a free PDF copy of the 112-page book at this link.
The excerpt below is adapted from the book’s chapter on active living.
The role of cardiac rehab
If you have had heart disease, a cardiac rehabilitation program teaches you how to safely become more active and make lifestyle changes so you improve your heart health and reduce your risk of future heart problems. Your cardiac rehab program team may include a:
- cardiologist
- nurse
- exercise professional
- dietitian
- psychologist
The team will help guide you toward heart health. Your family doctor can help to set you up with a program in your community. Find a cardiac rehab program close to you at cardiachealth.ca.
If you can’t find a cardiac rehab program in your community, you can help yourself by following the exercise program outlined in the book. Always check with your healthcare provider before beginning any physical activity program.
Just starting to exercise?
For many people, it is easy to start with walking. Below is an example of a walking program. Walk in the hallway, walk the length of your driveway, walk in the mall, walk a block, walk for 10 minutes.
Remember you are starting slow and easy. You may need to plan rest areas or places to stop and sit along the way. This program can be used for biking, stationary bike, water walking and swimming.
At home
Week 1
Every second day
Warm up:
Training period: 10-minute walk at
an easy pace
Cool down:
Week 2
Every second day
Warm up: 5-minute easy walk
Training period: 10-minute walk at a faster pace
Cool down: 5-minute easy walk
Week 3
4 times a week
Warm up: 5-minute easy walk
Training period: 15-minute walk at a faster pace
Cool down: 5-minute easy walk and stretches
Week 4
4 times a week
Warm up: 5-minute easy walk
Training period: 20-minute walk at a faster pace
Cool down: 5-minute easy walk and stretches
Weeks 5-6
At least 5 days a week
Warm up: 10-minute easy walk
Training period: 25-30 minute walk at a faster pace. Start to pump or swing arms. Walk up gentle hills, leaning slightly forward.
Cool down: 5-minute easy walk and stretch for each walk
A routine that fits your needs
As you progress, your cardiac rehab team can help you increase your activity slowly, steadily and safely, incorporating new activities you enjoy.
The FITT principle is a guideline to help you set up a workout routine that fits your goals and fitness level, while helping you get the most out of your exercise program. It helps you track and measure your progress.
FITT stands for:
- Frequency – how often? The goal is to exercise most days of the week.
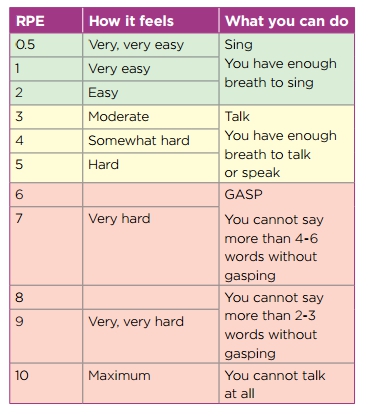
- Intensity – how hard? The rate of perceived exertion (RPE) is how hard you feel your body is working.
It is based on the way your body feels during exercise, including increased heart rate, breathing rate, sweating and muscle tiredness.
- Time – how long? Exercising 150 minutes each week is proven to be good for your heart health.
- Type – what kind?
- Aerobic or endurance exercise involves continuous movement of your large muscles (like your legs). It increases your breathing and heart rate, which improves your heart, lungs and circulatory system.
- Resistance exercise involves the development of muscle strength and endurance. Examples are lifting weights, using resistance bands and pushing or pulling your own body weight.
- Stretching or flexibility exercise keeps your muscles relaxed and your joints mobile.
Listen to your body
The best way to know if you are doing an exercise properly is to “listen to your body.” The following information can help you decide if the way you feel is normal or not.
During exercise it is NORMAL to feel:
- comfortable
- aware of your own breathing, but not out of breath
- slightly tired
- dry or slightly sweaty
- relaxed
During exercise it is NOT NORMAL to feel:
- chest pain (angina)
- dizzy or sick to your stomach
- short of breath, gasping
- very rapid or pounding heartbeat
- very sweaty or cold and clammy
- tense and nervous.
